
Is that inner knee pain just a minor tweak, or a sign of a serious ligament injury?
Many active people face this uncertainty. The medial collateral ligament, or MCL, is a common source of trouble. When it gets overstretched or torn, specific signs appear.
Localized pain on the inner side of the joint is a primary indicator. People often feel tenderness when pressing there. A sensation of the knee giving way or a popping sound at the moment of harm are also classic red flags.
Mass General Brigham Sports Medicine specialists provide expert evaluation for patients struggling with this instability. Getting a professional assessment is crucial for an accurate diagnosis.
Understanding these signals early helps prevent long-term problems. It ensures your recovery starts quickly. For instance, knowing how to approach managing an MCL sprain and squatting is vital for safe rehabilitation.
Key Takeaways
- Inner knee pain and tenderness are hallmark signs of an MCL issue.
- A feeling of instability or a “pop” often accompanies the injury.
- Seeking expert medical evaluation is essential for a correct diagnosis.
- Early recognition of symptoms can prevent further complications.
- Proper guidance is needed for activities like squatting during recovery.
- Swelling and bruising on the inside of the knee are common.
- Severe pain or trouble bending the knee warrants immediate attention.
Introduction and Overview of MCL Sprains
A strong band of tissue on the inner side of your knee provides crucial stability. This is the medial collateral ligament, or MCL. When it gets overstretched or damaged, we call it an MCL sprain.
Understanding the Role of the Medial Collateral Ligament
This ligament acts as your joint’s main defense against inward collapse. It connects your thigh bone to your shin bone. This prevents excessive side-to-side movement during daily activities.
The medial collateral ligament keeps your knee stable during running or jumping. Without it, your joint would buckle inward with each step. This makes it vital for athletes and active people.
Importance of Recognizing Symptoms Early
Spotting the first signs of trouble is essential. Early intervention prevents further damage to your knee joint. Ignoring initial pain can lead to chronic instability.
Timely recognition significantly improves your long-term prognosis. It helps avoid more invasive medical procedures later. As one sports medicine specialist noted,
“Catching an MCL issue early changes the entire recovery trajectory.”
Our overview explains why this ligament is frequently injured. We highlight how proper care starts with awareness. Knowing what to look for empowers you to take action quickly.
Anatomy and Function of the Medial Collateral Ligament
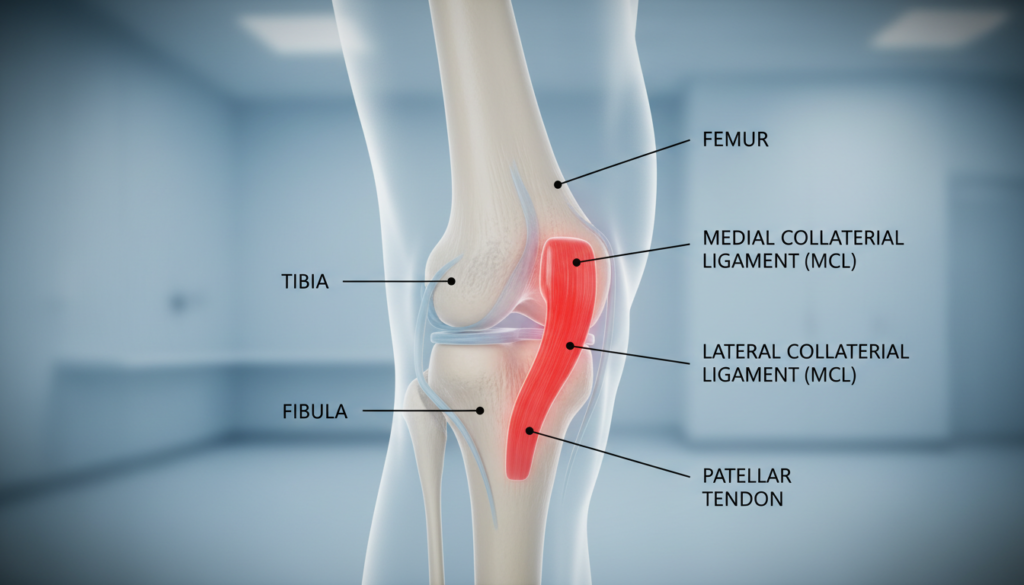
Understanding knee health begins with the anatomy of its most frequently injured ligament, the MCL. This band of tissue is involved in a staggering 40% of all reported knee joint injuries.
Structure and Location in the Knee Joint
The medial collateral ligament is a thick, strong band. It runs vertically along the inner side of your knee.
Anatomically, it stretches from the femur (thigh bone) down to the tibia (shin bone). This connection forms a vital structural support for the inner aspect of the joint.
How the MCL Stabilizes and Supports the Knee
This collateral ligament acts as a primary stabilizer. Its core job is to prevent the knee joint from buckling inward during movement.
It also limits excessive rotational forces. This maintains proper alignment during everything from walking to sports.
Because the MCL resists these common stresses, it becomes vulnerable. Knowing its specific location helps pinpoint where inner knee pain originates after an injury.
What are the symptoms of an MCL sprain?
A sudden pop followed by immediate inner knee tenderness signals a potential MCL problem. We will outline the key signs that differentiate this injury from general joint soreness.
Common indicators in pain and instability
The most frequent complaint is sharp pain localized directly over the ligament on the inner side. Many people report significant tenderness when touching that specific spot, which is a hallmark sign of an acute issue.
Instability is another frequent indicator. The joint may feel like it could buckle or give way during simple weight-bearing activities, such as walking or climbing stairs.
Bruising and swelling often accompany a significant mcl tear. These visual cues typically appear on the inner aspect of the knee within a day of the injury.
Recognizing these specific symptoms helps you understand the severity. It allows for a better-informed decision to seek professional medical attention for an accurate diagnosis of an mcl tear.
Grades of MCL Injuries
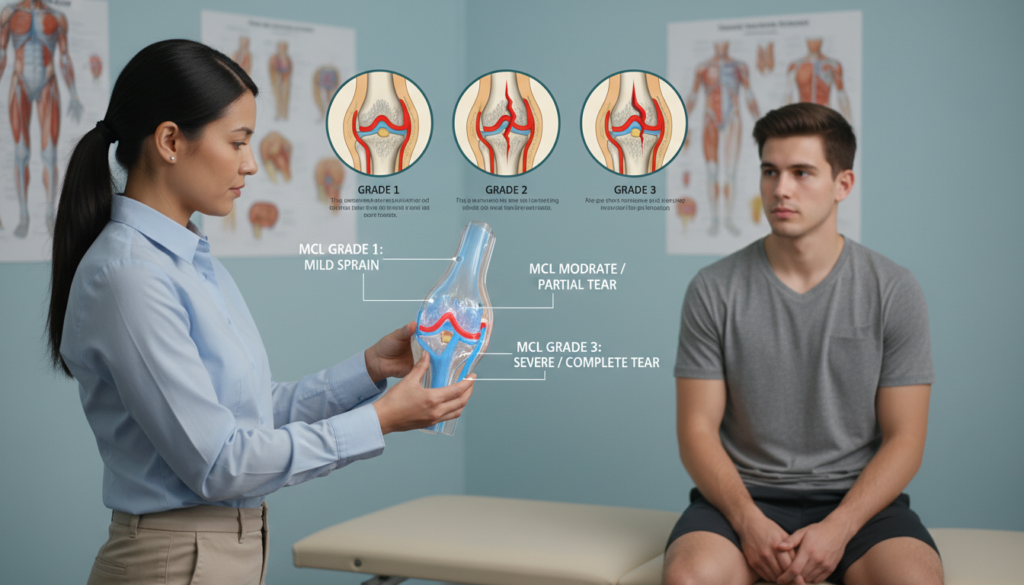
Not all MCL issues are the same. They range from minor stretches to full ruptures. Medical professionals use a grading system to classify the severity of the ligament damage.
This classification directly guides your treatment plan and recovery expectations. Knowing your grade is the first step toward a targeted rehabilitation strategy.
Grade I: Mild Sprain Characteristics
A Grade I injury is a mild sprain. The ligament fibers are overstretched but not torn.
You might feel some tenderness on the inner knee. Joint stability remains largely intact. With proper rest, this grade typically heals well within 1 to 3 weeks.
Grade II and Grade III: Partial and Complete Tears Explained
A Grade II mcl tear involves a partial rupture of the ligament. This causes moderate pain, noticeable swelling, and a sense of instability.
Recovery often takes 6 to 8 weeks. A Grade III tear is the most severe. It represents a complete rupture of the ligament fibers.
This grade causes significant knee instability and often requires up to 12 weeks or longer for full recovery. Higher-grade tears demand more intensive rehabilitation to restore strength and function.
| Grade | Description | Key Characteristics | Typical Recovery Timeline |
|---|---|---|---|
| Grade I | Mild Sprain | Ligament stretching, minimal instability | 1 – 3 weeks |
| Grade II | Partial Tear | Partial fiber rupture, moderate pain & instability | 6 – 8 weeks |
| Grade III | Complete Tear | Full ligament rupture, significant joint instability | 12+ weeks |
Accurate grading of an mcl tear is crucial. It determines the right path for healing your knee injury.
Causes and Risk Factors for MCL Sprains
Identifying what puts your knee at risk is crucial for preventing ligament injuries. Several common actions and conditions can lead to an MCL sprain.
Understanding these causes helps you avoid painful setbacks.
Sports-related and accidental impacts
High-impact sports are primary drivers of MCL damage. Football, soccer, and basketball involve frequent pivoting and direct contact.
Forceful side-impact collisions can stretch or tear the ligament. Accidental falls or poor landings during athletic activities also pose a significant risk.
These events often force the knee inward violently. The foot is usually planted, making the joint vulnerable.
Additional risk factors in daily activities
Beyond sports, daily tasks can strain the MCL. Heavy lifting or awkward squatting places cumulative stress on the inner knee.
This gradual damage weakens the ligament over time. Environmental factors like slippery surfaces contribute to the overall likelihood of a painful injury.
Specific movement patterns, as noted in a sports medicine review, increase susceptibility. Understanding these factors is the first step in prevention.
| Risk Category | Common Scenarios | Primary Mechanism | Prevention Tip |
|---|---|---|---|
| Sports & Contact | Football tackle, soccer pivot, basketball landing | Direct valgus force (knee bent inward) | Use proper technique and protective bracing |
| Accidental Trauma | Falls, missteps, awkward landings | Sudden twisting with foot fixed | Maintain balance and strengthen leg muscles |
| Daily Overuse | Heavy lifting, repetitive squatting | Cumulative micro-trauma to ligament | Practice proper body mechanics during tasks |
Diagnosing an MCL Sprain

Pinpointing the exact nature of your inner knee pain requires a combination of expert assessment and technology. A correct diagnosis ensures your treatment plan targets the specific ligament injury.
Your doctor will synthesize your history with clinical findings. This creates a clear path for your recovery.
Physical examination techniques and tests
A thorough physical exam is the cornerstone of diagnosis. Your doctor will first observe your gait and check for swelling.
They will then test the stability of your knee joint. A common technique is the valgus stress test.
Clinicians stabilize your femur while gently pushing your tibia outward. This assesses the integrity of the medial collateral ligament and checks for abnormal looseness.
Role of imaging: X-rays, MRI, and ultrasound
Imaging tools provide a deeper look inside the joint. Each modality serves a distinct purpose in evaluating an MCL injury.
An X-ray is useful first. It rules out fractures of the bones around the knee.
An MRI is often the preferred choice for soft tissue detail. It clearly visualizes the extent of an MCL tear and can reveal damage to other structures like the meniscus.
Ultrasound offers a rapid, dynamic assessment. It may be used for initial evaluation but typically provides less detail than an MRI for complex cases.
| Imaging Method | Primary Purpose | Best For | Limitations |
|---|---|---|---|
| X-ray | Rule out bone fractures | Initial screening | Cannot show ligament tears |
| MRI Scan | Detail soft tissue damage | Confirming MCL tear severity & associated injuries | More costly, less accessible |
| Ultrasound | Rapid, real-time assessment | Quick evaluation of ligament integrity | Operator-dependent, less detail for complex tears |
Consulting a qualified doctor is essential. They combine your history, the physical exam, and imaging results to create a personalized plan for your knee injury.
Treatment Options for MCL Sprains
Effective management of an MCL injury begins with a clear treatment plan. The chosen path depends heavily on the grade of your ligament damage.
Most cases heal successfully without an operation. Your doctor will recommend the best course for your specific knee issue.
Nonsurgical treatments: Rest, ice, and bracing
The gold standard for early care is the POLICE principle. This acronym stands for Protect, Optimal Loading, Ice, Compression, and Elevation.
Protection often involves using crutches to avoid weight-bearing stress. Optimal loading means gently moving the joint as pain allows.
Applying ice and compression wraps helps control swelling. Elevation keeps fluid from pooling around the injured knee.
Concurrently, remember the HARM protocol. Avoid Heat, Alcohol, Running, and Massage initially to prevent increased swelling.
This conservative treatment, including a supportive brace and adequate rest, restores full function for most people.
When surgery might be needed
Surgical intervention is less common. It is typically reserved for severe Grade III tears where the MCL is completely detached from the bone.
Your doctor might suggest you require surgery if other structures like the ACL or meniscus are also damaged. This combined injury often needs surgical repair for stability.
| Approach | Key Components | Typical Use Case | Expected Outcome |
|---|---|---|---|
| Nonsurgical Treatment | POLICE principle, bracing, HARM avoidance | Grade I & II MCL sprains, isolated injuries | Full recovery with restored stability |
| Surgical Treatment | Ligament repair/reconstruction | Grade III tears, multi-ligament injuries | Restored joint integrity, longer rehab |
Choosing the right treatment ensures your knee heals correctly. Always follow your medical provider’s guidance for your MCL recovery.
Recovery and Rehabilitation Process
Regaining full knee function after a ligament sprain requires a dedicated recovery process. We outline a structured program that adapts to your injury‘s severity.
This plan focuses on progressive exercises to rebuild stability. Consistent effort during this time is the key to a successful return.
Timelines Based on Injury Severity
Your healing schedule depends directly on the grade of your MCL damage. A clear timeline helps set realistic expectations.
| Injury Grade | Healing Focus | Typical Recovery Window |
|---|---|---|
| Grade I | Reducing inflammation, gentle mobility | 1 – 3 weeks |
| Grade II | Restoring stability, building muscle strength | 6 – 8 weeks |
| Grade III | Regaining full joint function post-surgery or severe tear | 3 months or more |
Patience during each phase prevents re-injury. Rushing back to sports can set your recovery back significantly.
The Role of Physical Therapy and Exercises
Targeted physical therapy is the most effective path forward. A therapist designs exercises for the quadriceps, hamstrings, and gluteal muscles.
Strengthening these supporting structures protects the healing MCL. It restores the knee‘s natural stability.
Dedication to your prescribed routine is the primary method for restoring full range of motion. This consistent work ensures you return to activities with confidence, minimizing the time lost to your injury.
Prevention Strategies and Strengthening Exercises
The best defense against a sidelining knee injury is a consistent focus on prevention and muscle conditioning. We focus on practical habits that build resilience in the medial collateral ligament.
Integrating these strategies into your routine minimizes future risk. It keeps you active and performing at your best.
Warming Up and Proper Training Techniques
A dynamic warm-up is non-negotiable before any athletic activity. It increases blood flow and prepares your muscles and ligaments for the demands of the game.
This simple practice significantly reduces strain on the MCL. Proper training technique is equally vital.
Learning to land softly with bent knees after a jump is essential. It distributes force safely away from vulnerable ligaments.
Strengthening the quadriceps and hamstrings is a proven method for protection. These muscles act as dynamic stabilizers for your knee joint.
“Conditioning the lower body provides a protective buffer for the medial collateral ligament. It’s the most effective insurance policy an athlete can have.”
Dedicating time to these exercises improves overall joint stability. A consistent routine builds the strength needed during sports.
| Prevention Focus | Key Actions | Primary Benefit |
|---|---|---|
| Dynamic Warm-up | Leg swings, light jogging, mobility drills | Prepares tissues, reduces initial strain on MCL |
| Strength Training | Squats, lunges, hamstring curls | Builds muscle support to stabilize the knee |
| Technique Practice | Plyometric landing drills, agility work | Teaches safe movement patterns to avoid traumatic injury |
By focusing on these strategies, you safeguard your MCL. This proactive approach helps maintain performance all season long.
Considerations for Athletes and Active Lifestyles
Competitive sports place immense rotational forces on the knee, making a robust MCL essential for athletes in football and similar activities. For them, an MCL tear is not just a medical issue; it’s a career challenge demanding a specialized approach.
We explore the unique options and protocols designed for a high-performance comeback.
Managing Knee Stability During Sports
High-impact pivoting and direct contact constantly test ligament integrity. To withstand this, professional athletes often opt for surgery to repair a significant MCL tear.
This ensures the joint can handle the intense demands of their sport. Reconstruction surgery may involve using a tissue graft from the hamstring tendon.
This graft replaces the damaged ligament to restore native stability. It’s a common solution when the original MCL fails to heal strongly on its own.
Guidance on Returning to Activity Safely
Coming back from an MCL tear requires official medical clearance. This is especially critical if you have also suffered an associated ACL injury.
A safe transition back to sport ensures the knee tissue is fully healed and capable of handling stress. Rushing this process risks re-injury and longer setbacks.
For many active individuals, the decision to require surgery is based on restoring peak performance. The goal is to prevent long-term instability in the knee.
A comprehensive diagnosis and treatment plan is the foundation. It’s also vital to differentiate your injury from other issues, like a meniscus tear.
| Decision Factor | Description | Implication for Athlete |
|---|---|---|
| Severity of Tear | Grade III complete tears often need surgical repair for stability. | Longer rehab but higher likelihood of returning to pre-injury level. |
| Associated Injuries (e.g., ACL) | Combined ligament damage complicates healing and stability. | Surgery is frequently recommended to address all damaged structures at once. |
| Sport Demands | Sports with cutting, jumping, and contact place high valgus stress on the knee. | May push the decision toward surgical intervention for robust, reliable healing. |
| Surgical vs. Non-Surgical Outcome | Surgery aims for anatomical restoration; non-surgical care relies on scar tissue formation. | Athletes often choose surgery for a more predictable return to high-level function. |
Conclusion
Your journey back to full activity after a medial collateral issue hinges on informed decisions and consistent care. We have outlined the common symptoms an MCL injury presents and the various treatment paths available for recovery.
Understanding the anatomy of your knee‘s collateral ligament complex is vital for any patient. Whether managing minor tears or recovering from significant damage, consistent treatment is the key to restoring your quality of life.
We hope this guide has clarified the differences between various grades of tears. Professional medical guidance remains essential for a safe and effective outcome.
By prioritizing your rehabilitation and following expert advice, you can successfully return to favorite activities in due time.
