You feel a sharp pop on the inner side of your leg. Suddenly, your joint feels unstable. For many active people, this moment starts a journey filled with one pressing question.
Our team at Mass General Brigham Sports Medicine understands this uncertainty. We see patients grappling with the decision between invasive procedures and conservative care every day.
To find clarity, you must first understand the anatomy. The medial collateral ligament (MCL) is a critical band of tissue. It connects your thigh bone (femur) to your shin bone (tibia) on the inner knee.
A complete tear of this ligament is a serious event. It can drastically affect your ability to walk, pivot, or bear weight. The path to healing depends on many personal factors.
This guide breaks down the latest clinical evidence. We help you navigate the complex choices for long-term joint health and stability. Our goal is to empower your recovery, whether you’re a professional athlete or enjoy weekend activities.
Key Takeaways
- The medial collateral ligament (MCL) is a key stabilizer on the inner side of the knee joint.
- A complete, or grade 3, tear is a severe injury that challenges joint stability.
- Many complete ligament tears heal successfully without an operative procedure.
- The decision for surgical intervention depends on the injury’s specifics and your activity goals.
- Professional evaluation is crucial to assess damage and create a personalized treatment plan.
- Non-surgical management often involves bracing, physical therapy, and a structured rehab program.
- Long-term outcomes focus on restoring strength, function, and confidence in the joint.
Overview of Grade 3 MCL Sprain
The medial collateral ligament is one of the most commonly injured structures in the knee. This overview explains its critical role and the spectrum of damage it can sustain.
Understanding the Medial Collateral Ligament Anatomy
This key band of tissue connects your thigh bone, or femur, to your shin bone, the tibia, on the inner side. It acts as a primary stabilizer, preventing excessive side-to-side movement of the knee joint.
Differences Between Grade 1, 2, and 3 Injuries
We categorize the severity of these mcl injuries on a scale. A mild injury involves only stretched fibers. A complete rupture, however, means all ligament fibers are torn.
Healing timelines reflect this difference. Mild cases may resolve in weeks. A full tear often needs three months or longer. Research shows nearly 78% of patients with a complete medial collateral ligament tear have damage to another knee structure.
Proper identification is essential for effective treatment and a strong recovery.
Does grade 3 MCL sprain require surgery?
Determining the best path forward after a severe ligament injury hinges on a careful comparison of approaches. It is not a simple yes-or-no answer.
Our team evaluates each case individually. We weigh the potential for natural healing against the benefits of an operative procedure.
Comparing Nonsurgical and Surgical Treatment Options
A key reason many full ligament tears heal without an operation is excellent blood supply. This natural healing potential is a major advantage.
Persistent instability during daily tasks is a crucial factor. If the knee feels loose and unreliable, surgical repair may be considered.
| Treatment Approach | Primary Goal | Ideal Candidate | Key Considerations |
|---|---|---|---|
| Nonsurgical Care | Support natural healing and restore function | Isolated tear with good healing response | Involves bracing, dedicated physical therapy, and a phased rehab program. |
| Surgical Intervention | Mechanically restore stability | Complex injury with multiple damaged structures | Reserved for cases where the ligament fails to heal on its own over time. |
| Clinical Decision | Personalized recovery plan | All patients | Balances risks of an operation with the patient’s specific activity goals and anatomy. |
We typically reserve surgery for complex situations. These include injuries where other knee structures are also damaged.
Consulting with a specialist is essential. They can determine if your specific injury requires a surgical repair for optimal long-term joint health.
Symptoms and Diagnostic Criteria for MCL Tears
Diagnosing a full-thickness ligament rupture relies on both patient-reported symptoms and clinical evaluation. We combine these elements to form a complete picture of the damage.
Common Signs: Pain, Swelling, and Instability
People often feel a sharp pain on the inner side of the knee immediately after the event. Significant swelling typically follows within hours.
A telling symptom is a feeling of instability, as if the joint might give way. Many also recall hearing a distinct “pop” sound at the moment of injury.
Diagnostic Tools: Physical Exams and MRI
Our physical exam includes the valgus stress test. This maneuver assesses the ligament‘s integrity by applying pressure to the outer knee.
To confirm a suspected mcl tear and check for other damage, we often use magnetic resonance imaging (MRI). This scan provides detailed visuals of soft tissues like the ligament and meniscus.
These criteria help us distinguish a simple strain from complex tears. Accurate diagnosis guides the right treatment plan for your knee injury.
Causes and Risk Factors for MCL Injuries
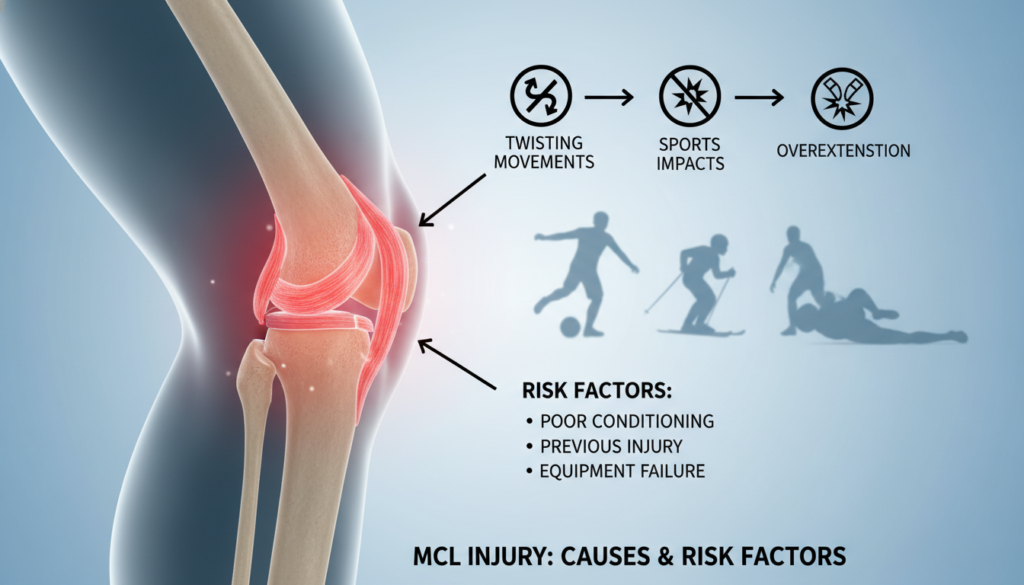
A direct blow to the outer knee remains the most common culprit behind medial collateral ligament tears. High-impact sports like football, soccer, and basketball are primary drivers of these mcl injuries due to rapid changes in direction and collisions.
Most damage occurs when a force hits the outer side of the knee, pushing the joint inward. This motion stretches the ligament beyond its normal limit, resulting in a tear. The sudden, forceful impact we see in our practice is a classic mechanism for this type of injury.
Athletes involved in these sports face a higher risk. Constant jumping, sprinting, and pivoting place extreme stress on the joint. Changing direction quickly while running can overload the knee‘s stabilizers.
Understanding these risk factors is crucial for prevention, especially for competitive players. Proper conditioning and awareness of body mechanics can help mitigate danger. If you’re wondering about mobility after such an injury, learn more about your ability to walk with a torn MCL.
Non-Surgical Treatment Options for MCL Sprains
Our first priority after a complete tear is to control symptoms and create an optimal healing environment. Many severe ligament injuries heal successfully without an operation. We focus on proven methods that support the body’s natural repair processes.
Rest, Ice, Compression, and Elevation (RICE)
The RICE protocol is our gold standard for initial care. It involves four key steps: rest, ice, compression, and elevation. This approach directly addresses pain and reduces swelling in the first critical days.
We emphasize complete rest from impact to allow the damaged tissue to begin healing. Applying ice regularly helps manage discomfort and inflammation. Using a compression wrap or a specialized knee brace provides needed support.
Role of Physical Therapy and Bracing in Recovery
A well-fitted protective device safeguards the joint during early movement. It offers stability while the ligament regains strength. This external support is crucial for preventing re-injury.
Guided physical therapy forms the core of long-term recovery. Our therapists design exercises to restore mobility and build muscle around the knee. This tailored therapy helps patients safely return to their active lifestyles.
Our non-surgical treatment plans combine these elements for a comprehensive approach. Consistent care and progressive exercises foster a strong, functional recovery.
Surgical Treatment: When and Why It May Be Needed
Persistent knee instability despite thorough rehabilitation is a primary indicator for surgical evaluation. We recommend this path only when a patient’s specific anatomy and goals align with the benefits of an operative repair.
Indications for Surgery in Grade 3 Injuries
Our team considers a surgical procedure for complete ligament tears when the joint remains loose. This often happens with complex multi-ligament damage or when a person is a high-demand athlete.
Key factors include the location of the tear and the quality of the native tissue. The final choice is always personalized, balancing risks with the patient’s desired activity level.
Surgical Techniques and Procedures Overview
If the tissue is repairable, we perform a direct repair. This involves suturing the torn ends back to the bone to promote healing.
For poor-quality tissue, we use a graft to reconstruct the ligament. This graft can come from the patient’s own body (autograft) or a donor (allograft).
Modern techniques often use a mini-open approach. This method can reduce recovery time and improve outcomes.
Surgical recovery typically takes 6 to 8 weeks. The exact timeline depends on the complexity of the repair and the individual’s healing response. For a deeper look at this decision process, we guide patients through determining if MCL surgery is right for.
Recovery Timelines and Rehabilitation Strategies
The road back to full activity after a complete medial collateral ligament tear demands patience and a phased approach. We establish clear expectations from the start.
Recovery time varies significantly with the severity of the knee injury. General timelines include:
- Mild injuries: Often heal within 3 to 4 weeks.
- Moderate tears: Typically require 6 to 8 weeks of recovery time.
- Severe ruptures: Can take 12 weeks or longer, depending on the individual.
Our rehabilitation strategies prioritize two goals: gradually rebuilding knee strength and minimizing joint stiffness. We progress exercises in stages that match your tissue’s healing phases.
Following a structured plan is essential. It ensures the damaged ligament regains its capacity to stabilize the knee during movement.
Our physical therapists manage this process closely. They ensure you do not return to high-impact sports too soon, which risks re-injury.
Consistent monitoring over these weeks is vital for long-term knee health. We adjust your program based on progress and feedback.
Managing Pain and Swelling Post-Injury

Controlling post-injury symptoms is a critical step for a comfortable recovery journey. We prioritize this management to help patients remain at ease during the initial healing phase.
Effective Home-Care Methods and Medications
Simple home-based strategies make a significant difference. Icing the affected area for 20-minute intervals reduces inflammation and discomfort effectively.
Keeping the leg elevated above heart level decreases swelling. This common symptom can limit your range of motion after ligament tears.
Over-the-counter medications like NSAIDs help manage pain and inflammation in the knee joint. Always use them under professional guidance for safety.
Consistent application of these methods improves the patient experience. It creates a better environment for the body’s natural repair processes to work.
Preventative Measures for Avoiding Re-Injury
The best defense against a recurring knee injury is a strong offense built on targeted conditioning and smart training habits. We focus on proactive strategies that empower your joint for long-term health.
Strengthening the leg muscles is a cornerstone of our approach. Powerful quadriceps and hamstrings act as natural stabilizers, reducing strain on the MCL during activity.
Strengthening and Conditioning Techniques
We advocate for comprehensive programs that go beyond basic exercises. Proper training techniques teach your body to move efficiently, lowering risk during athletic performance.
Wearing a supportive knee brace during high-impact drills can provide extra stability. This external support helps prevent the joint from buckling under stress.
Physical therapy exercises that focus on balance and agility are essential. They improve proprioception, so your knee reacts better to sudden shifts in direction.
A thorough warm-up prepares the muscles to absorb forces. Dynamic stretches increase blood flow and flexibility around the knee.
Our tailored preventative programs maintain the strength and flexibility your knee needs. We build a foundation that keeps you active and confident, helping to avoid future medial collateral ligament tears.
Expert Insights and Clinical Recommendations
Drawing from years of clinical practice, we’ve learned that every medial collateral ligament case tells a unique story. Our recommendations are built on this deep, hands-on experience treating active individuals from all walks of life.
Our Experience with MCL Injury Treatments
Dr. Prem N. Ramkumar, our orthopedic specialist in Long Beach, emphasizes a foundational step. “A meticulous physical exam is non-negotiable for every patient,” he notes. This exam assesses the specific ligament damage and overall knee stability.
We treat each MCL injury with a plan tailored to the person’s anatomy and goals. This personalized approach considers lifestyle, activity demands, and the precise nature of the injury. Early, focused intervention for a severe tear often leads to stronger long-term outcomes.
Our team provides specialized care for those dealing with a painful medial collateral ligament problem. We serve patients from Los Angeles and Orange County, ensuring they access advanced clinical recommendations close to home.
Clear dialogue about the risks and benefits of any surgery is essential. We believe informed patients make the best decisions for their recovery. For a deeper look at evolving treatment protocols, current research offers valuable perspectives.
Recent Advances in MCL Injury Research and Treatment
Cutting-edge research is reshaping how we approach complex ligament damage in the knee. New studies provide crucial insights for optimizing recovery from a complete tear.
A landmark 2018 analysis in EFORT Open Review revealed a critical pattern. It highlighted that 95% of associated injuries in severe cases involve the ACL. This finding underscores the need for comprehensive evaluation of every mcl injury.
We are now better at identifying when an mcl problem coincides with an ACL tear. This changes our surgical strategy significantly. Advances allow us to better repair the ligament to the bone, improving stability.
New evidence suggests the quality of the native tissue is a major factor. It determines the success of a primary repair for these tears. Our clinical practice actively incorporates these latest findings.
We ensure every patient receives the most effective, personalized care for their knee. This commitment to research-driven treatment leads to stronger, more reliable outcomes after a significant injury.
Conclusion
Your journey back to full mobility after a severe knee injury hinges on a well-informed, personalized strategy. While a complete ligament tear is serious, many achieve excellent results through dedicated physical therapy and proper care.
Surgery is a vital option for those with complex ligament injuries or persistent instability. We strongly encourage consulting a specialist to map the best path for your joint health and goals.
Recovery demands patience and consistent effort, often spanning several weeks. This time is essential for rebuilding strength and stability in the knee.
By following expert guidance and focusing on preventative conditioning, you can protect your knee and confidently return to the activities you love.
