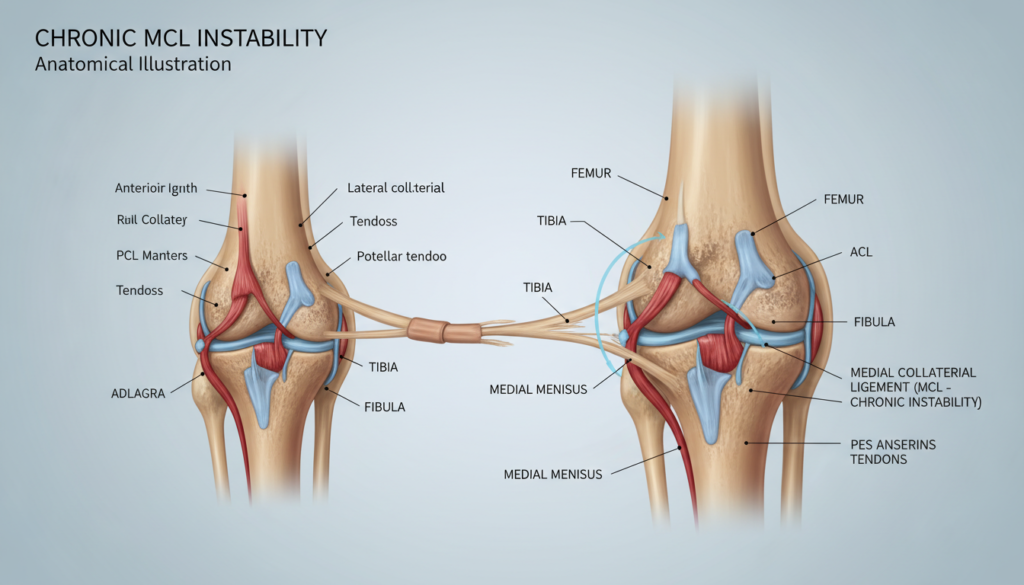
Why does a seemingly healed knee injury keep causing your joint to buckle during simple activities? This frustrating experience is common for many active people.
We define this persistent problem as a condition where the medial collateral ligament fails to provide adequate support after initial trauma. The ligament on the inner side of your knee becomes unable to control sideways motion.
Research shows these knee injuries are frequent. Studies report an annual incidence ranging from 0.24 to 7.3 cases per 1,000 people. Men experience this issue twice as often as women.
Patients often feel their knee give way during sports or when changing direction. This sensation is a hallmark of ongoing instability. It signals that the primary stabilizer against inward buckling is compromised.
Proper diagnosis is crucial. Experts use tools like the valgus stress test to assess joint laxity. Imaging, such as an MRI, helps confirm the extent of damage to the ligament and surrounding structures.
Understanding the difference between a fresh injury and a lingering one is vital for effective care. Correct management protects your long-term joint health and function. For many, following specific physical therapy protocols for MCL forms the cornerstone of recovery.
Key Takeaways
- Chronic MCL instability is a persistent condition where the knee’s inner ligament fails to provide stability after an initial injury.
- The annual incidence of medial collateral ligament injury ranges from 0.24 to 7.3 per 1,000 people, with men affected more than women.
- A key symptom is the sensation of the knee “giving way,” especially during sports or changes in direction.
- Diagnosis typically involves a physical valgus stress test and often imaging like an MRI to evaluate the damage.
- Distinguishing between acute and chronic cases is essential for determining the correct treatment and management plan.
- Left unaddressed, this instability can lead to persistent pain and limit an active individual’s function.
- Proper evaluation looks at the entire knee joint, including the collateral ligament and joint line, to prevent long-term issues.
Understanding the Medial Collateral Ligament (MCL)
The inner side of your knee houses a crucial band of tissue that acts as your joint’s primary defense against buckling inward. This structure, the medial collateral ligament, is the most common ligament injured during knee trauma. We must grasp its role to understand why certain injuries are so prevalent.
Role in Knee Stability
This collateral ligament serves as the main stabilizer against valgus forces. These are stresses that push the knee inward. During running or cutting, the MCL prevents excessive sideways motion. It works alongside the anterior cruciate ligament for complex stability.
Relevance in Ligament Injuries
Because of its position, the medial collateral ligament is frequently damaged in contact sports. A direct blow to the outer knee is a typical cause. Athletes often report immediate swelling and tenderness along the inner joint line.
Proper evaluation uses the valgus stress test to assess damage. Imaging like an MRI helps grade the tear. Early diagnosis guides effective management. This often includes bracing and targeted physical therapy to restore strength.
Anatomy and Biomechanics of the MCL
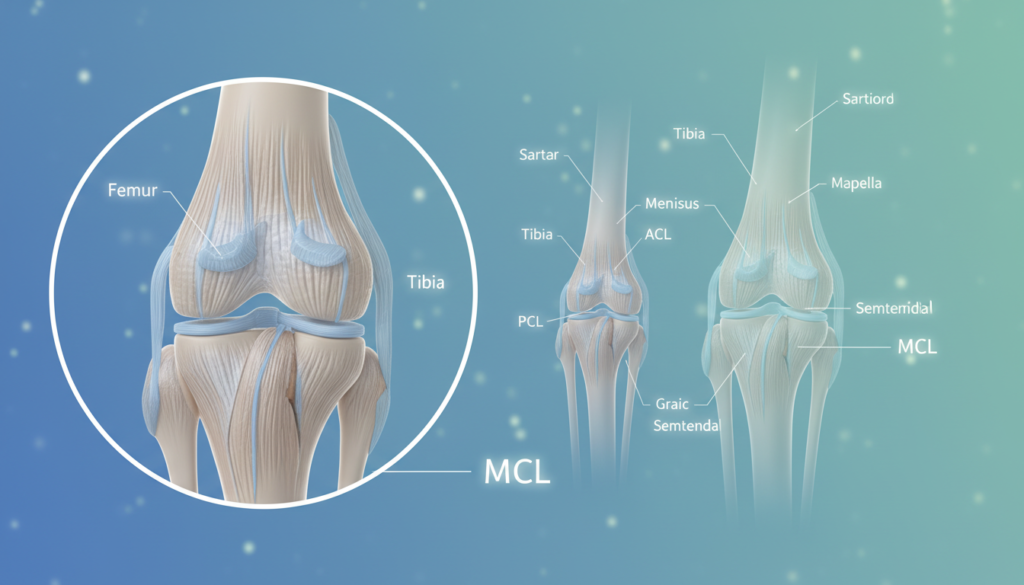
The medial collateral ligament isn’t a single band but a layered structure that provides multi-directional support to the knee. We examine its detailed design to understand how damage occurs.
Superficial and Deep MCL Structures
The superficial medial collateral ligament is the primary restraint. It originates 3.2mm proximal and 4.8mm posterior to the medial femoral epicondyle bone.
This attachment point is critical for controlling inward motion. The deep part of the collateral ligament has two arms.
These are the meniscofemoral and meniscotibial arms. They anchor the medial meniscus to the joint capsule.
| Structure | Origin/Attachment | Primary Function |
|---|---|---|
| Superficial MCL | Medial Femoral Epicondyle | Resists Valgus Stress |
| Deep MCL (Meniscofemoral) | Femur to Meniscus | Stabilizes Medial Meniscus |
| Deep MCL (Meniscotibial) | Meniscus to Tibia | Controls Joint Line Motion |
The Posteromedial Corner and POL
The posteromedial corner includes the posterior oblique ligament. It acts as a secondary stabilizer during rotation.
The semimembranosus muscle tightens this corner. This action prevents anterior subluxation of the tibia.
Understanding this biomechanics is vital for diagnosis and treatment. The valgus stress test assesses these structures.
Proper management of collateral ligament injuries prevents long-term issues. The anterior cruciate ligament works with the MCL for full knee protection.
What is chronic MCL instability?
Repetitive stress from sports like soccer can gradually stretch the medial collateral ligament, leading to lasting instability. This condition often stems from many small injuries over time or a tear that healed poorly.
We see soccer players are prone to these knee problems. The kicking motion places constant stress on the inner ligament. This can cause increased joint looseness, known as valgus laxity.
A key sign on MRI is a wavy, elongated appearance of the collateral ligament. This classic finding confirms long-term damage. The valgus stress test is also crucial for diagnosis.
This physical test can reveal excess laxity even without sharp pain. It assesses the collateral ligament knee complex. Persistent swelling or tenderness along the inner joint line warrants a doctor’s visit.
Proper management of these cases is vital. It prevents further wear on the joint. The anterior cruciate ligament may also suffer in chronic instability.
Understanding this progression helps athletes choose the right treatment. It guides a safe return to sports. Early intervention stops long-term degeneration.
| Feature | Acute MCL Injury | Chronic MCL Instability |
|---|---|---|
| Primary Cause | Single traumatic event | Repetitive microtrauma or healed injury |
| Pain Level | Often severe and immediate | May be minimal or absent |
| Swelling | Significant acute swelling | Persistent, low-grade swelling |
| MRI Finding | Clear tear or disruption | Wavy, elongated ligament appearance |
| Valgus Stress Test | Painful with endpoint laxity | Painless with increased laxity |
Correct management of collateral ligament injuries protects your knee’s future. Imaging like an MRI provides a clear picture. We advise professional evaluation for any lingering knee issue.
Mechanisms and Causes of MCL Injuries
The mechanisms behind medial collateral ligament damage range from high-force contact to subtle, repetitive strains. Most MCL injuries happen during active sports like soccer, skiing, or ice hockey.
A direct blow to the outer knee applies a valgus force. This stress pushes the joint inward, overloading the inner ligament. Contact sports frequently produce this mechanism.
Non-contact knee injuries are also common. Awkward landings or sudden changes in direction can strain the collateral ligament. An athlete plants a foot and twists, placing significant stress on the tissue.
Repetitive microtrauma leads to gradual ligament degradation over time. This is a key cause of chronic issues for professional athletes. The anterior cruciate ligament is often involved in these cases, complicating management.
| Mechanism Type | Primary Force | Common Sports | Typical Injury |
|---|---|---|---|
| Direct Contact | Valgus Stress (side impact) | Football, Ice Hockey | Acute Grade II-III Tear |
| Non-Contact | Rotational/Deceleration | Soccer, Basketball | Grade I-II Sprain |
| Repetitive Overuse | Microtrauma | Running, Cycling | Chronic Ligament Laxity |
Proper diagnosis requires a thorough physical exam. The valgus stress test assesses collateral ligament injuries. Early recognition of these injuries prevents long-term knee instability.
Clinical Presentation and History of MCL Instability
The clinical story of a knee injury provides essential clues for an accurate diagnosis and effective treatment plan. We gather this information by listening carefully to the patient and observing specific physical signs.
Symptoms and Patient History
Patients with a medial collateral ligament injury typically report localized swelling, ecchymosis, and tenderness on the medial side of the knee. This bruising and pain are hallmarks of acute damage.
We note that the timing of the physical exam is critical. Muscle spasms can mask the true extent of the collateral ligament damage if assessment is delayed.
A detailed history often reveals a specific trauma. This could be a direct collision or a sudden change in direction during sports. Our team evaluates the entire collateral ligament knee complex to differentiate isolated injuries from those involving the anterior cruciate ligament.
We discuss how the valgus stress test identifies laxity in the medial collateral ligament, even in longstanding cases. Proper management begins with understanding the patient’s symptoms and the initial injury mechanism.
We emphasize that tenderness along the inner joint line is a key indicator. Our guide helps clinicians interpret this presentation to ensure accurate diagnosis and effective planning.
Physical Examination and Valgus Stress Testing
The valgus stress test provides direct feedback about the medial collateral ligament‘s condition. We perform this manual assessment to check the knee‘s inner stability.
It is the primary tool for evaluating suspected collateral ligament injuries. Our team relies on its findings to plan effective treatment.
Interpreting Laxity and Pain
We perform the test with the knee bent to 30 degrees. This position isolates the medial collateral ligament from other structures.
Applying a gentle inward force, we look for medial laxity. Observed looseness is a key sign of ligament damage. Comparing the injured side knee to the healthy one is crucial for an accurate diagnosis.
If instability appears when the knee is fully straight (0 degrees), it suggests a more severe injury. This often means the anterior cruciate ligament or other structures are also involved.
For complex cases, we use additional tests. The Slocum test identifies anteromedial rotatory instability. The dial test helps differentiate damage to the posterolateral corner.
These findings guide our clinical decisions. They tell us if the ligament has a partial tear or a complete rupture.
| Physical Exam Test | Knee Position | Positive Finding | Clinical Implication |
|---|---|---|---|
| Valgus Stress Test | 30° Flexion | Medial Joint Laxity | Isolated MCL Injury |
| Valgus Stress Test | 0° Extension | Gross Laxity | Possible ACL/PCL Involvement |
| Slocum Test | 90° Flexion, Foot Externally Rotated | Anteromedial Tibial Subluxation | Severe Medial Ligament Injury |
| Dial Test | 30° & 90° Flexion | Increased External Tibial Rotation | Posterolateral Corner Injury |
Proper management starts with this careful exam. Interpreting the stress response and pain location directs the next steps. A reliable assessment prevents missed injuries and supports a full recovery.
Medical Imaging and Diagnostic Techniques
Advanced imaging tools provide a window into the structural integrity of the knee’s inner stabilizer. We use these techniques to confirm a diagnosis and plan effective treatment.
Accurate visualization is crucial for proper management of collateral ligament injuries.
Radiographic Evaluation
Radiographic evaluation starts with standard X-rays. Anteroposterior weight-bearing views help identify bone avulsions or calcifications.
The Pellegrini-Stieda sign is a key finding. This calcification near the medial femoral epicondyle suggests a prior medial collateral ligament injury.
Stress radiography can quantify joint looseness. It measures the medial joint space opening under a valgus stress test force.
This confirms the extent of damage to the collateral ligament knee complex.
MRI Assessment and Grading Correlations
Magnetic resonance imaging offers detailed soft tissue views. We utilize MRI to visualize the medial collateral ligament directly.
It allows for precise grading of the tear. A grade I injury shows increased signal intensity on T2-weighted sequences.
A grade III tear indicates complete ligament disruption. Our team notes a high agreement between MRI and clinical grading for these knee injuries.
This imaging helps surgeons plan for potential reconstruction in severe cases. It also identifies associated injuries to the anterior cruciate ligament.
| Imaging Modality | Primary Use | Key Finding | Clinical Implication |
|---|---|---|---|
| X-ray (AP Weight-bearing) | Detect bone abnormalities | Pellegrini-Stieda sign | Suggests chronic medial collateral injury |
| MRI (T2-weighted) | Visualize soft tissue damage | Increased signal intensity | Indicates grade I ligament tear |
| Stress Radiography | Quantify joint laxity | Increased medial joint space opening | Confirms collateral ligament instability |
Integrating these findings with the physical exam provides a comprehensive diagnosis. This guides all subsequent management steps.
Grading and Classification of MCL Injuries

A standardized grading system helps doctors categorize the severity of damage to the knee’s inner stabilizer. This classification is essential for planning the correct treatment path.
The American Medical Association defines three primary grades for these ligament injuries. Each grade describes a different level of tissue disruption.
Clinical Grading vs. Radiographic Grading
Clinical grading relies on a physical exam. The valgus stress test assesses joint looseness and pain.
This method is subjective but remains a cornerstone in sports medicine. It provides immediate feedback during the patient visit.
Radiographic grading uses advanced imaging like MRI. It offers a detailed view of the ligament’s structure.
There is often high agreement between these two approaches. Our team compares both to ensure an accurate diagnosis.
Researchers like Hughston further divided severe cases. They looked at the amount of medial knee space opening under stress.
| Grade | Clinical Findings (Valgus Stress) | Radiographic/MRI Findings | Management Implication |
|---|---|---|---|
| Grade I | Minimal laxity, firm endpoint | Increased signal, minimal fiber damage | Conservative therapy, bracing |
| Grade II | Partial laxity, soft endpoint | Partial tear visible | Protected motion, strength exercises |
| Grade III | Complete laxity, no endpoint | Complete ligament disruption | Possible surgical repair |
Proper classification of the collateral ligament injury guides all subsequent steps. It helps clinicians decide between non-surgical care and an operation.
This framework is vital for predicting recovery time. It sets clear expectations for athletes and active individuals.
Conservative Management and Rehabilitation Strategies
Non-surgical care forms the foundation for healing most injuries to the knee’s inner ligament. Our approach focuses on early protected motion to prevent stiffness and support natural healing.
We initiate gentle range motion exercises soon after the injury. This practice maintains joint health and guides collagen alignment.
For more severe cases, a hinged brace provides crucial support. Grade II injuries typically require this support for three weeks. Grade III ligament damage often needs six weeks of bracing.
Strengthening the surrounding muscles is vital. We emphasize quadriceps exercises like straight leg raises. These exercises stabilize the knee during daily activities.
Structured physical therapy guides the return to sports. It ensures proper loading time and movement patterns. Most isolated medial collateral ligament problems heal well with this treatment.
Our management of collateral ligament injuries follows a clear progression. We monitor each phase to confirm healing.
| Rehabilitation Phase | Primary Focus | Typical Duration |
|---|---|---|
| Protection & Pain Control | Reduce swelling, use brace | Weeks 1-2 |
| Early Motion & Strengthening | Restore range, begin quad sets | Weeks 3-6 |
| Advanced Strengthening | Build strength for sports | Weeks 7-12 |
| Return to Activity | Sport-specific drills, full function | Months 3-4 |
This stepwise plan helps athletes regain confidence. Consistent follow-up ensures the knee is ready for demands.
Surgical Options and Timing Considerations
A Stener-type lesion, where the ligament is displaced, is a clear mandate for surgical management. We also consider an operation when conservative care fails to restore adequate stability.
Direct Repair vs. Reconstruction
Direct repair is typically chosen for acute injuries. This approach reattaches the torn ends of the ligament when the tissue quality is still good.
For chronic ligament injuries with poor tissue, reconstruction is the preferred method. This procedure uses tendon grafts to rebuild the damaged structure and restore knee function.
Combined Injury Management
Staged management is often needed for complex multi-ligament knee injuries. We carefully plan the timing to address each damaged part.
When both the anterior cruciate ligament and the medial collateral ligament are injured, they may be repaired or reconstructed in a single procedure. Early range motion exercises after surgery are crucial to prevent stiffness.
Modern techniques, like internal brace augmentation, provide extra support during healing. Our team tailors the surgical plan to the specific grade of injury and the patient’s goals.
MCL Instability in Athletes and Chronic Implications
Soccer players face a unique risk for lingering knee problems due to the biomechanics of kicking. The repetitive stress places constant valgus force on the inner ligament. This can lead to a gradual stretch and persistent laxity over time.
Without proper management, these injuries cause long-term functional deficits. Specialized rehabilitation addresses the persistent looseness and pain. It focuses on dynamic strength and stability training for the entire knee.
Chronic MCL issues often affect the anterior cruciate ligament and overall joint health. Early diagnosis is key to stopping this cascade. It prevents secondary damage and more complex cases.
| Athlete Risk Factor | Essential Management Strategy |
|---|---|
| Repetitive Valgus Stress (e.g., Soccer) | Biomechanical Analysis & Technique Modification |
| High-Grade Ligament Tear | Extended Protective Bracing & Phased Strength Program |
| Associated ACL Injury | Coordinated Surgical & Rehab Planning |
| Demands of High-Level Competition | Multidisciplinary Sports Medicine Team Approach |
Our team emphasizes a multidisciplinary approach for athletes. Sports medicine experts design plans to maintain knee strength and prevent re-injury. Proper management of the collateral ligament knee complex ensures a safe return to sports.
Prevention, Screening, and Return to Play Guidelines
Screening protocols are a frontline defense against misdiagnosed knee laxities. Regular checks by team physicians can spot pre-existing looseness in the ligament. This helps prevent future knee injuries.
Preventing medial collateral ligament damage involves specific training. Neuromuscular programs teach proper landing and cutting mechanics. Strengthening the hip and core muscles also reduces stress on the inner knee.
Return to sports should rely on objective strength and stability tests. The passage of time alone is not enough. We must also assess the anterior cruciate ligament before clearing athletes for contact.
Our management includes a gradual return to activity. This ensures the collateral ligament knee complex is fully prepared. Monitoring for signs of lingering instability stops injuries from recurring.
| Prevention Strategy | Key Action | Target Outcome |
|---|---|---|
| Regular Screening | Valgus stress test by team physician | Identify pre-existing ligament laxity |
| Neuromuscular Training | Focus on landing and cutting mechanics | Reduce risk of knee injuries |
| Strength Conditioning | Strengthen hip and core muscles | Decrease stress on medial collateral ligament |
| Return-to-Play Protocol | Objective strength and stability tests | Ensure safe return to sports |
Coaches and trainers play a key role. Implementing these strategies protects athletes and promotes long-term knee health.
Long-Term Outcomes and Future Treatment Directions
Regular check-ups ensure that a healed ligament continues to provide stability for years. Long-term results for these knee problems are generally positive. Patients must stick to their rehab and strength programs.
Maintaining strong quadriceps muscles protects the joint from wear over time. The anterior cruciate ligament also plays a key role in lasting stability after a medial collateral tear.
Future treatment is moving toward biological therapy. These methods aim to improve the body’s own healing for ligament injuries. Advancements in sports medicine are shaping this new path.
Our team emphasizes patient education. It is crucial for the best outcomes in lingering cases. Consistent therapy and early range motion exercises form a solid recovery foundation.
Periodic reassessment keeps the collateral ligament knee complex stable. New research on ligament healing supports these practices.
| Factor for Success | Key Action | Long-Term Benefit |
|---|---|---|
| Rehabilitation Adherence | Complete strength program | Restored knee function |
| Quadriceps Strength | Regular strengthening exercises | Protection from joint degeneration |
| Follow-up Frequency | Periodic clinical assessment | Early detection of laxity |
| Use of Advanced Therapies | Adoption of biological treatments | Improved ligament healing quality |
Proper management of these injuries leads to a full return to sports. We look forward to more innovations in knee care.
Conclusion
Successfully managing knee ligament damage requires a clear roadmap and consistent effort.
Our exploration highlights the need for accurate diagnosis and tailored management of medial collateral injuries. Understanding the knee’s biomechanics is essential for assessing severity.
Structured rehabilitation, including strength exercises, restores function after a tear or persistent laxity. This training also safeguards the inner side of the joint from future problems.
Keeping pace with sports medicine progress leads to optimal outcomes. This guide provides a comprehensive resource for overcoming these challenges and ensuring lasting joint health.
