What if the path back to the game depends more on smart rehabilitation than just waiting it out?
This question is at the heart of every athlete’s mind after a knee setback. The medial collateral ligament is a band of tissue connecting your thigh bone to your shin bone. It stabilizes the inner knee during side-to-side motion.
When this ligament is overstretched or torn, it results in an MCL injury. Common signs include pain on the inner side of the leg, noticeable swelling, and a feeling of the knee giving way.
These symptoms signal that the joint’s stability is compromised. Proper management from the start is crucial. It prevents long-term joint damage or chronic instability.
Our team at the Southern California Orthopedic Institute emphasizes early evaluation for any medial collateral ligament issue. We know that asking when can I return to sports after MCL sprain? is a top concern.
The answer is never one-size-fits-all. It hinges on the specific grade of your MCL injury. A detailed rehabilitation pathway is essential for a safe and strong comeback.
Key Takeaways
- The medial collateral ligament is a key stabilizer on the inner side of the knee.
- MCL injuries often cause inner knee pain, swelling, and a sense of instability.
- Early and proper management is vital to prevent long-term joint problems.
- Recovery time depends heavily on the specific grade of the ligament sprain.
- A structured rehab program is the cornerstone of a successful return to activity.
- Professional evaluation guides the safest and most effective recovery plan.
Understanding the Medial Collateral Ligament and MCL Injuries
Athletes in contact sports like football frequently experience MCL injuries due to direct forces applied to the knee’s inner side. Understanding this ligament is key to grasping the nature of these common knee problems.
Function and Importance of the MCL
The medial collateral ligament is a band of tissue running along the inner side of your knee. It connects your thigh bone to your shin bone. Its primary job is to prevent excessive side-to-side movement, providing crucial stability.
When this collateral ligament is damaged, the knee loses a major source of support. This often leads to feelings of instability during activity.
Common Types and Grades of MCL Injuries
We categorize these ligament injuries into three distinct grades. This system helps us plan the right treatment.
A grade 1 injury is a mild sprain with slight stretching. A grade 2 tear is a partial rupture causing more pain. A grade 3 injury is a complete tear of the collateral ligament.
Severe MCL injuries often involve other structures. A grade 3 mcl injury may occur alongside an anterior cruciate ligament tear. The ACL and MCL are stressed by similar forces.
Fortunately, the medial collateral tissue has a good blood supply. This aids the natural healing process and influences the recovery path. Proper classification of these collateral ligament injuries guides our medical intervention.
When can I return to sports after MCL sprain?

Mapping out your comeback from a knee ligament injury requires clear timelines and tailored treatment plans.
Recovery Timelines Based on Injury Severity
Healing time for these ligament injuries varies greatly by grade. A mild grade 1 sprain often allows a return in 1-2 weeks.
More significant grade 2 tears typically need 3-4 weeks. Research, like a 2013 UEFA study of 346 cases, supports this timeline for minor ligament issues.
A complete grade 3 tear demands patience. Recovery often spans 6 to 8 weeks or longer.
For athletes, the exact recovery time hinges on rehab dedication and sport-specific demands.
Non-Surgical Versus Surgical Treatment Options
We choose the right treatment by assessing the tear’s severity and the knee’s stability.
Non-surgical care is the gold standard for most isolated MCL injuries. It combines rest, activity modification, and a hinged brace.
Consistent physical therapy rebuilds strength and confidence during this period.
Surgery is rare for a simple collateral ligament injury. It may be necessary if the anterior cruciate ligament is also torn.
Operative repair is also considered if the knee joint shows persistent instability after non-surgical care.
Our goal is always to restore full stability before clearing you for full-contact activity.
Rehabilitation Strategies and Best Practices

A strategic rehab plan is the bridge between a knee injury and a confident return to play. Successful recovery blends immediate protective care with progressive, targeted exercise.
Bracing, Rest, and Icing Techniques
Initial treatment focuses on managing pain and swelling. We use the RICE method—rest, ice, compression, elevation—as a foundation.
A hinged knee brace is often prescribed. It provides external stability, shielding the healing medial collateral ligament from unwanted stress.
This protection is crucial for the first few weeks, especially for higher-grade tears.
Physical Therapy and Gradual Activity Progression
Structured physical therapy sessions then take the lead. They rebuild the quadriceps and hamstrings, which are vital secondary stabilizers.
We guide a gradual progression. It starts with simple range-of-motion movements. Later, it advances to strength and balance drills.
This controlled activity rebuilds confidence while protecting the collateral ligament. Monitoring progress ensures milestones are met safely.
Tailoring Recovery to Your Specific Sport
Rehab must match your sport’s demands. The cuts in basketball stress the knee differently than the pivots in soccer.
We design sport-specific drills late in the recovery phase. For severe cases requiring surgery, we coordinate closely with surgeons.
Our goal is a full, functional return. Understanding your detailed recovery timeline helps set realistic expectations for your comeback.
Diagnosis, Imaging, and Specialist Evaluation
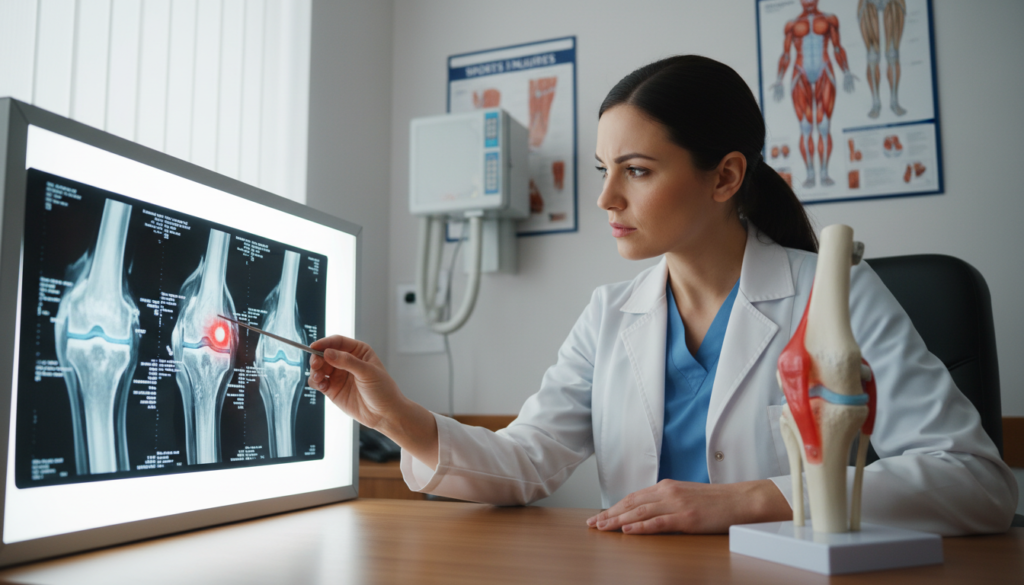
Determining the true severity of a medial collateral ligament injury requires a multi-faceted diagnostic approach. A precise evaluation is the first critical step toward effective care.
Physical Exams and the Role of MRI in Evaluation
A sports medicine specialist begins with a hands-on physical exam. The valgus stress test applies pressure to the outer side of the knee to check for inner joint laxity and instability.
This exam assesses the integrity of the collateral ligament. It also helps identify any associated meniscus or bone injuries.
Advanced imaging, like an MRI, is often the next step. It provides a detailed picture of the soft tissues. The scan confirms the grade of the ligament injury and can rule out damage to the ACL.
Identifying Risk Factors and Warning Signs
We listen for specific warning signs during the patient history. A loud “pop” sensation or immediate inability to bear weight on the injured leg often signals a severe tear.
Understanding risk factors is part of our medicine practice. Poor landing mechanics or playing on uneven surfaces increase the chance of ligament injuries.
Early evaluation by a sports medicine expert is crucial. Untreated collateral ligament injuries can lead to long-term joint issues and chronic pain.
An accurate diagnosis ensures your treatment plan, including tailored physical therapy protocols, is built for your specific recovery goals.
Exercise Guidelines and Therapy for a Safe Return to Sports
The transition from healing to high-performance hinges on precise strengthening and sport-specific retraining. Our therapy plans are designed to rebuild dynamic stability and confidence in the knee.
Essential Strengthening and Balance Exercises
Strengthening the quadriceps and hamstrings is non-negotiable. These muscles absorb stress that would otherwise strain the healing medial collateral ligament.
We integrate balance drills to improve proprioception. This is vital for preventing non-contact ligament injuries in sports like football.
Sport-Specific Drills and Activity Modification
Activity modification maintains fitness during the healing weeks. Low-impact exercise protects the collateral ligament while preserving cardiovascular health.
Later, we design drills that mimic your sport’s demands. This ensures your knee can handle cuts, pivots, and jumps. Passing functional tests for agility and instability is a final milestone.
For those who needed surgery, recovery includes specific structured rehabilitation protocols. Consistent therapy guides a safe progression back to play.
Conclusion
Your journey back to peak performance concludes with a focus on long-term joint health and confidence. Recovering from an MCL injury demands patience and a structured approach. This ensures the medial collateral ligament heals with full stability.
Whether managing a mild injury or rehabilitating after surgery, expert guidance is key. Working with a sports medicine professional provides the safest path forward. They tailor your treatment and activity progression.
Listen to your body and prioritize your knee health. Persistent pain or instability warrants a conversation with your care team. A successful recovery builds a solid foundation for all future athletes.
